New paper in Bioessays on the toolkit to capture intraspecific variation in metabolic rate4/12/2023 How do we capture variation in metabolic rate within and among species? I am excited about our new Bioessays paper (led by Neil Metcalfe & Pat Monaghan) that examines this important question. This publication stems from the Rank Prize Symposium on "Variation in Metabolic Rate: where does it come from and does it matter?" in July 2022. I unfortunately contracted covid-19 on day 1 of the conference and spent its entirety attending virtually from my room. So I was thrilled to take part in the group effort to write this opinion piece! Thanks to my unfortunate buddy in covid quarantine, Amelie Crespel, with whom I worked on my section and one of the tables. Check out the paper here: https://onlinelibrary.wiley.com/doi/full/10.1002/bies.202300026 
0 Comments
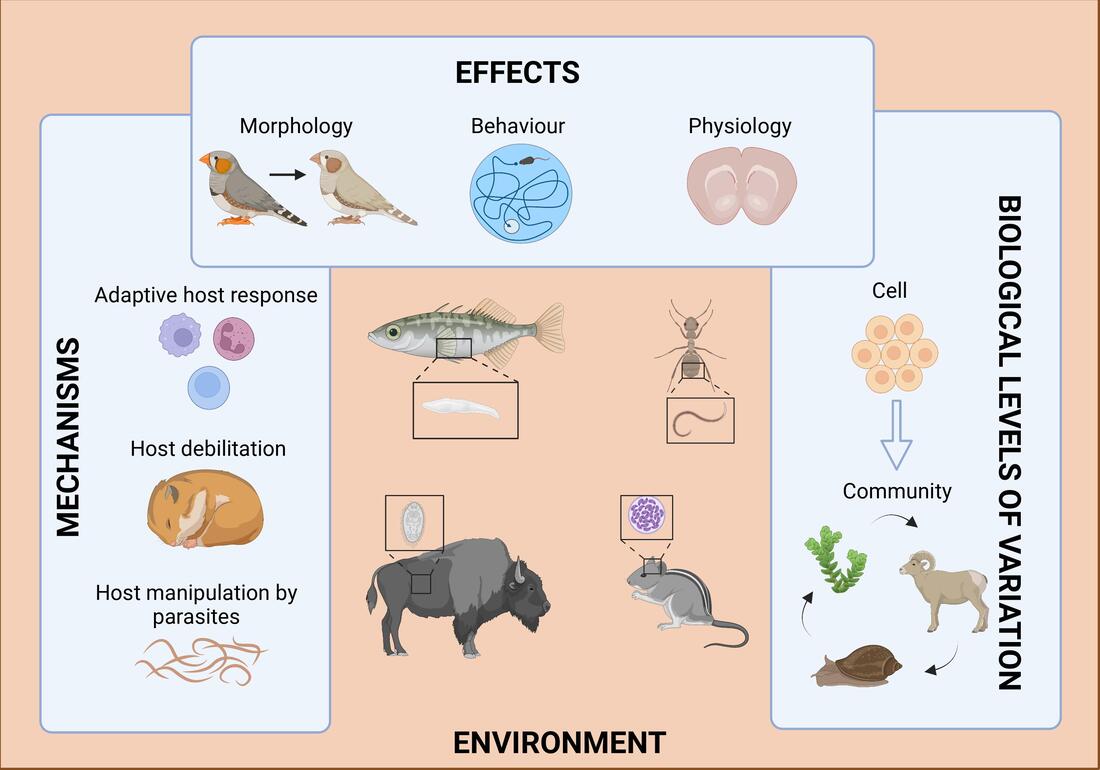
After nearly 2 years, I am thrilled to see the cross-journal special feature in Functional Ecology and Journal of Animal Ecology that we guest-edited out now, focused on mechanisms and consequences of infection-induced phenotypes. Check out all of the amazing contributions here: https://besjournals.onlinelibrary.wiley.com/toc/13652435/2023/37/4. The graphical abstract from our editorial included below!
After endless packing, I am excited to be officially here at the University of Southampton. I had an amazing (and breezy) introduction to the Solent right at the waterfront campus' doorstep with other new lecturers on the RV Callista. More to come soon!
After three weeks in the field in Australia, we have returned from the first annual field "Transdisciplinary approaches to coral reef science" course, funding by the National Science Foundation's International Research Experiences for
Students track II program. We learned a ton that we can use to make the course even better in the future and think the students had an amazing experience as well. I am excited to announce that the NMBP lab is moving to the University of Southampton in the UK in fall 2022. I will be based at the National Oceanography Centre. This unique location on the south coast of England will allow access to the many unique marine systems close by and facilitate collaborations with the many amazing researchers at the University and close by.
After a year of pandemic induced delays, I finally have fish (and snails) in my lab! Yayyy! The fish species in the lab are Fundulus similis (longnose killifish) and F. grandis (gulf killifish). Both are known second intermediate hosts for the Euhaplorchis sp. A parasite, which is found on their brain. They are infected by free-swimming larval parasites called cercariae that depart the first intermediate host, Cerithideopsis scalariformis (ladder hornsnail). With both the first and second intermediate host in the lab, I will be able to do experimental infections of the killifish to determine how they response (either behaviorally or physiologically) to these infectious parasites in their environment. I studies a closely related system in California, and found that the killifish host wasn't happy when it encountered cercariae in their environment and am interested in testing similiar ideas here.
FUNDULUS! After a couple of failed missions to find Fundulus spp. killifish, I found the little buggers finally this past weekend. I worked with a related species in California, examining how parasites alter their behavior, and my goal is to develop a local system to continue that work. Step 1 was to find a reliable place to collect them, which I did last weekend at Spruce Creek in New Smyrna Beach, FL. Check! ☑️ First few fish already dissected with the my collaborator Chris Blanar and our students.
 It took a few years but the last (and arguably coolest!) chapter from my PhD was published today in the journal Communications Biology. In this study, we tested how the long-lasting social bonds associated with familiarity impact anti-predator behavior (known as the fast-start response) in a schooling coral reef fish, Chromis viridis (pictured to the left, photo credit Amy Cox). In social animals living in the wild, individuals rely on their buddies to alert them if a predator is lurking, but they need to balance the risk of being eaten against the wasted energy of reacting to inaccurate information. So, individuals will alter their sensitivity to social information based on the level of familiarity in the group (and hence trust in the information’s accuracy). Through greater trust in social information, familiarity thus maximizes the benefits of group living, for example, by minimizing aggression, enhancing cooperation, and increasing lifespans. In this study, we showed that familiar groups react more quickly and with greater speed following a simulated predator attack than groups composed of unfamiliar individuals. These effects were driven by a combination of greater vigilance by the first fish to detect the predator (also known as the response initiator) and more effective information sharing with neighboring fish. As escape performance underpins survival of predator attacks, these results help us to understand why animals have evolved to prefer associating with “friends” rather than “strangers”, due to the implications for both individual and group-level survival in the wild. Check out the paper here: https://www.nature.com/articles/s42003-021-02407-4 |
Archives
April 2023
Categories |








 RSS Feed
RSS Feed